Get PrEPped! Tips for Giving Your Sexual Health Toolbox a Glow Up
By Kristin Kennedy, Li Lock, and Adrian Neil Jr. | July 20, 2022
HIV & Sexual Reproductive Health at ETR
In July of 2012, the FDA (Food and Drug Administration) approved Truvada® for PrEP, pre-exposure prophylaxis. While this advancement was a huge breakthrough in HIV prevention, many health equity barriers still exist for clients/patients that prevent PrEP from becoming an accessible and engaging aspect of their sexual health.
As public health and health education professionals, we still have a lot of work to do and we can’t do it alone. We’re excited to share this resource with you to help your teams:
- Explore barriers to PrEP use such as stigma and lack of comprehensive PrEP education
- Discuss the new and different types of PrEP (e.g., injections and on-demand use)
- Expand PrEP and healthcare access for young people
- Review other tools clients/patients can use in their sexual health toolbox
PrEP and HIV-related Stigma
Despite the excitement around the momentous breakthrough of PrEP, we were — and still are—faced with cultural and medical stigmas against those who choose to use PrEP. Some have experienced being called derogatory names such as “PrEP whore.” In other cases, physicians have refused to prescribe PrEP either because they were not properly trained on what PrEP is, or because prescribing a drug that will empower people to engage in the type of sex and pleasure they want is outside of their comfort zone and conflicts with their personal beliefs.
During an interview with The Body Pro, psychologist Sarit Golub stated:
“…something that I have talked about in other venues is sort of the psychological tragedy of the HIV epidemic—the extent to which folks were taught to associate the act of sex, in and of itself, and especially condomless sex, with fear of HIV transmission.
In some ways, even the empowerment that emerged from activism had a certain tinge to it that said something like, ‘We’re going to embrace our sexuality and we’re going to embrace sex positivity, but we have to acknowledge that there’s always this thing kind of hanging over us, and that sex positivity and that sexual expression has to come with a cost.’’’
In order for us to effectively educate communities on HIV prevention and change the cultural landscape that surrounds PrEP, public health professionals must eradicate the stigma that is associated with being sexually empowered.
Understanding Different Types of PrEP
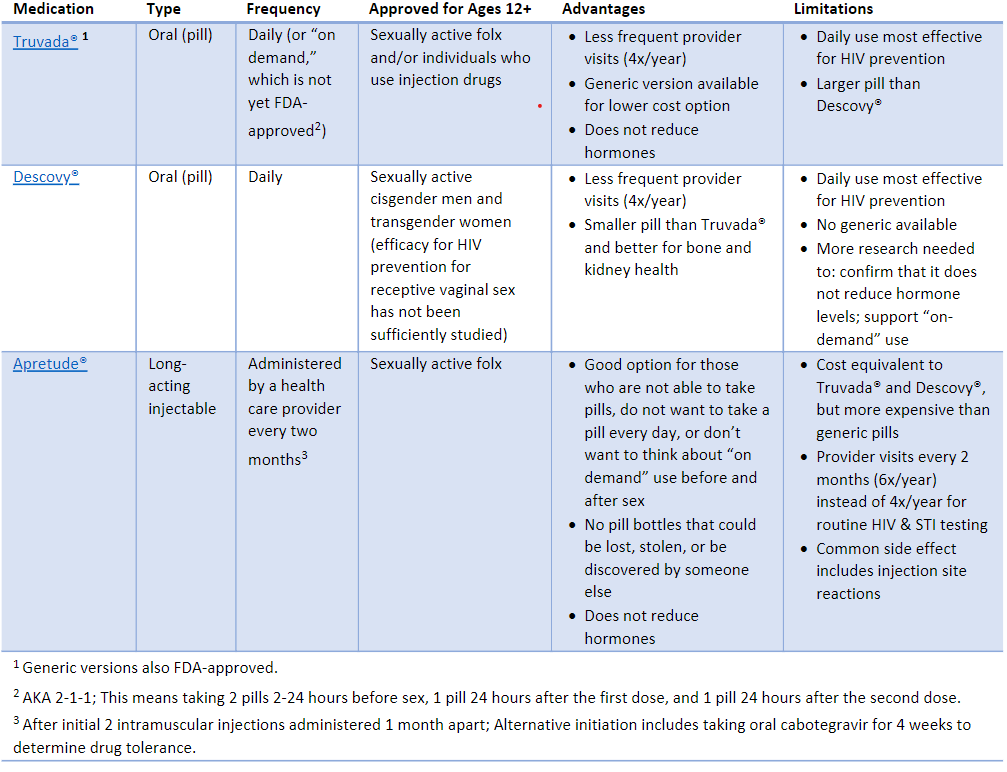
There are currently two FDA-approved daily oral pills for PrEP and a new long-acting injectable form of PrEP, all of which contain HIV antiretroviral (ARV) medications. If used consistently and correctly, the following types of PrEP medication can reduce the chance of getting HIV by up to 99%.
Expanding Access to PrEP for Young People
Data shows that only about 16% of young people ages 16-24 for whom PrEP is recommended were prescribed it in 2020, making this population the least likely to be using PrEP. Innovative strategies are essential for engaging and retaining young people in sexual health programs/services, including the use of PrEP for HIV prevention.
A few solutions to previously noted barriers for young people include offering digital health services and drop-in provider visits, implementing social media-based and peer-led interventions, incorporating adherence tools and appointment reminders, and providing navigation support with insurance coverage and PrEP access programs.
Continuing to offer new and different ways of taking PrEP medication may be a strategy for improving uptake among youth. While not yet FDA-approved, “on-demand” or 2-1-1 dosing of PrEP has been endorsed by the World Health Organization and the International AIDS Society-USA as an effective HIV prevention option for individuals who engage in anal sex less frequently or who are unable to or prefer not to take daily PrEP. Potential modalities include topical products delivered as gels, rings, films, and long-acting/extended-release (LA/ER) systems such as microneedles and implants. These are still in early development but could increase access and uptake, as more choices increase the chances of reaching a wider youth audience.
Sexual Health Toolbox for HIV Prevention
In addition to PrEP, there are many other tools you can help youth identify as part of their sexual health toolbox for HIV prevention:
- Knowledge: There is a lot of misinformation about HIV out there, so learning what HIV is, how it works in the body, and how it is transmitted and treated, can go a long way -- plus you can correct others and help stop the spread of misinformation that feeds HIV stigma!
- Testing: HIV testing is the only way to know your status, and knowing your status enables you to make informed decisions about your health. Everyone should get tested at least once in their life, and many people can benefit from testing more frequently – once per year, every six months, every three months, and/or with each new partner. Testing can be scary, but no matter whether your result is reactive or nonreactive, there are actions you can take to stay healthy and well. Testing is typically free or low cost and available through health departments, sexual health clinics, and many medical providers—there are also kits to test yourself! To find a testing site near you, visit https://gettested.cdc.gov/ or use the tool at the bottom of this page.
- Communication with partners: Talk about testing, share your results with one another, and discuss what you’re both/all comfortable with doing. You can even get tested together! Consent is sexy and sharing test results is a major part of consent. The ability to be open, honest, and unafraid to discuss HIV and other STIs is also a sign of trust – an absolute must for consent.
- Exploring different types of sex: Because of how fluids are exchanged, some types of sexual contact have a lower likelihood of HIV transmission, like kissing, touching, mutual masturbation, and oral sex (if there are no open wounds or sores).
- Barrier methods: If the bodily fluid from a person living with HIV never comes into contact with a mucous membrane or the bloodstream of a person without HIV, it won't be transmitted! Methods that provide a physical barrier between one person’s fluids and a partner’s body include internal and external condoms, dams, gloves, and finger cots. Barrier methods also minimize the risk of pregnancy and the transmission of STIs like chlamydia, gonorrhea, syphilis, human papillomavirus (HPV), and herpes simplex virus (HSV).
- Syringe services: For people who inject drugs, programs that provide a range of services such as access to sterile syringes and injection equipment, testing, and linkage to treatment can minimize HIV transmission through shared needles. Find a syringe service program near you: https://www.nasen.org/map/
- PEP: if there is a potential exposure, there's always post-exposure prophylaxis, or PEP. PEP is a medicine that stops HIV from replicating in the body. PEP should be taken within 72 hours after a potential exposure to HIV whether through sex or sharing needles. You can find PEP near you using the tool at the bottom of this page.
Additional PrEP Resources
You can also utilize these resources to support your community with accessing PrEP:
ETR Store: ETR’s HIV education materials address both prevention and treatment issues for a range of audiences and ages served by public health programs, schools, colleges, private medical providers, community-based organizations, and the military.
PrEPTECH: PrEPTECH is a paid study to see if an online program will help people who aren't already on PrEP start and continue taking it.
Ready, Set, PrEP: The Ready, Set, PrEP program provides free PrEP HIV-prevention medications to thousands of people living in the United States, including tribal lands and territories, who qualify.
PrEP Watch is a one-stop site for PrEP data, research, cost, access, implementation, and advocacy efforts across the globe.
State PrEP Assistance Programs: Some state PrEP assistance programs also cover clinical visits and labs.
ViiVConnect offers a program to help pay for Apretude® PrEP shots.
Gilead's Advancing Access® Program is committed to helping you afford Truvada® and Descovy® no matter your situation.

